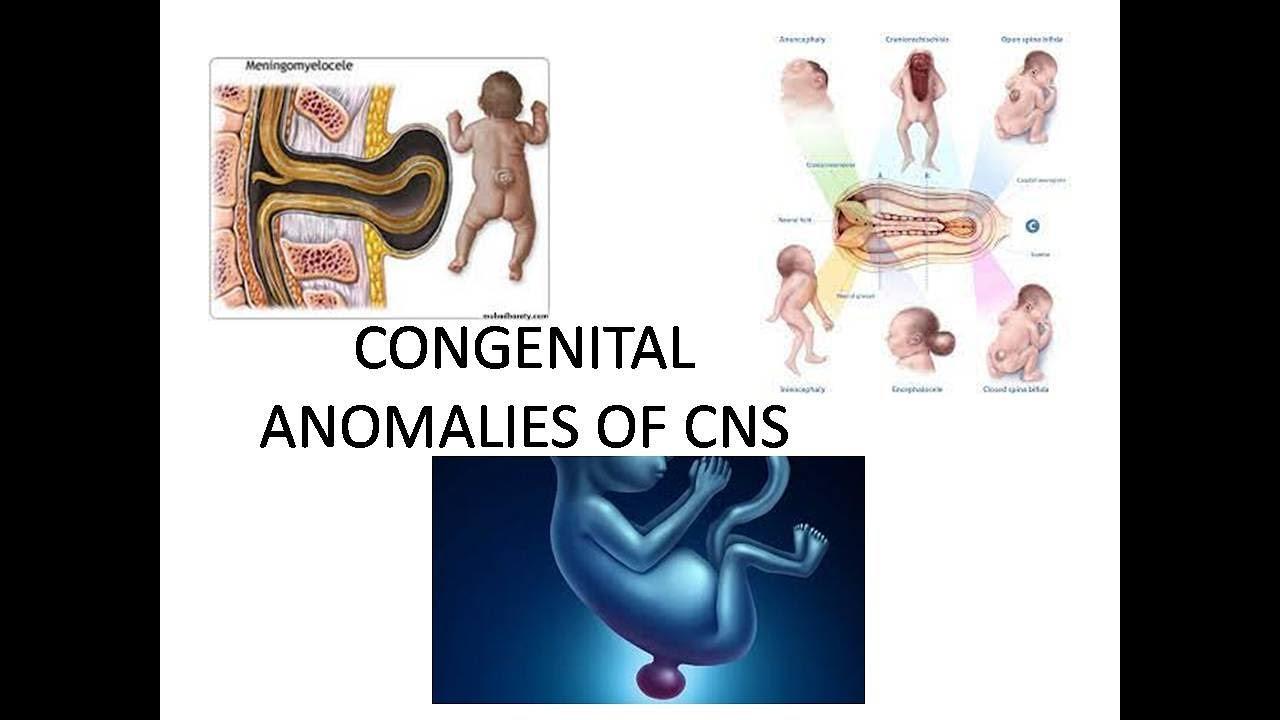
Specialized Post-Operative Care for Infants Following Corrective Surgery
1. Hemodynamic and Metabolic Stabilization
The immediate post-operative window (the first 24 to 72 hours) is focused on maintaining "homeostasis"—the body’s internal balance.
-
Fluid and Electrolyte Precision: Infants have a limited renal (kidney) capacity to handle excess fluid. Specialized "micro-infusion" pumps are used to deliver intravenous fluids with milliliter-level accuracy, ensuring the heart and kidneys are not overloaded while the body recovers from anesthesia.
-
Thermal Regulation: Maintaining a "neutral thermal environment" is critical. Because infants lose heat rapidly, especially in climate-controlled medical facilities, they are often placed in double-walled isolettes. This prevents "cold stress," which can deplete the infant’s energy reserves and slow down the cellular repair of the surgical site.
-
Nutritional Support: Depending on the surgery (especially for gastrointestinal or cardiac anomalies), infants may receive Total Parenteral Nutrition (TPN). This bypasses the digestive system to deliver essential amino acids and lipids directly into the bloodstream, providing the "building blocks" needed for tissue regeneration.
2. Multi-Modal Pain and Sedation Management
Modern pediatric care follows a "comfort-first" philosophy. Uncontrolled pain in infants can lead to increased heart rates and metabolic stress, which hinders healing.
-
Non-Pharmacological Comfort: Techniques such as "Kangaroo Care" (skin-to-skin contact with parents) and "sucrose dipping" are used to trigger natural endorphin release.
-
Regional Nerve Blocks: Whenever possible, surgeons perform long-acting nerve blocks during the procedure. This "numbness" can last for 12 to 24 hours post-surgery, allowing the infant to wake up calmly without the need for high doses of systemic opioids.
-
Scheduled Analgesia: Rather than waiting for the infant to show signs of distress, pain medication is often given on a strict schedule. This "prevents the peak" of pain, leading to a smoother recovery and earlier discharge.
3. Advanced Wound Care and Scar Stabilization
For Congenital Anomalies in Riyadh, the external aesthetic result is as important as the functional repair. The local environment plays a significant role in how a scar matures.
-
The "Moist Wound Healing" Principle: Modern incisions are never left to "air out." They are covered with advanced hydrocolloid or silicone-based dressings. This prevents the formation of a hard scab, which can act as a mechanical barrier to new skin cells (keratinocytes) migrating across the wound.
-
Tension Off-Loading: To prevent a scar from widening as the infant moves, "Steristrips" or medical-grade skin glues (Dermabond) are used to provide a secondary layer of support. These act as an external scaffold, taking the pressure off the delicate suture line.
-
Silicone Therapy Initiation: Once the initial incision has closed (usually at day 10–14), specialized silicone gel sheets are applied. Silicone works by increasing the hydration of the scar tissue, which signals the body to stop producing excess collagen, preventing "raised" or hypertrophic scars.
Comparison of Recovery Milestones
| Recovery Phase | Primary Goal | Monitoring Focus | Duration |
| Acute (NICU) | Stability | Vital signs; Fluid balance. | 1 to 5 Days |
| Sub-Acute (Ward) | Function | Feeding; Pain control. | 5 to 10 Days |
| Early Maturation | Tissue Integrity | Wound healing; Infection check. | 2 to 4 Weeks |
| Long-Term Remodeling | Aesthetic Blending | Scar softening; Growth tracking. | 6 to 18 Months |
4. The "Riyadh Factor": Environmental Shielding
The arid and sun-intensive climate of the region necessitates specific post-operative safeguards to protect the infant’s "new" skin.
-
Aggressive Photo-Protection: Immature scar tissue lacks melanin and can burn or darken (hyperpigmentation) in seconds under the Saudi sun. For the first year, any surgical site must be covered by UPF 50+ clothing or thick physical sunblocks (Zinc Oxide) whenever the child is outdoors.
-
Hydration and Humidity: Because dry air can cause skin to itch and pull, parents are advised to use high-quality, fragrance-free emollients around the surgical site (but not on the fresh incision) to maintain skin elasticity.
-
Dust and Allergen Control: In the dusty environment of the city, keeping the surgical dressings clean is paramount. Parents are taught "sterile technique" for home dressing changes to prevent environmental bacteria from entering the healing wound.
5. Parental Integration and "Home-Care" Transition
The final stage of specialized care is empowering the parents to become the "primary caregivers" of the surgical site.
-
The "Teach-Back" Method: Before discharge, parents must demonstrate they can safely clean the wound, administer oral medications, and recognize the "red flags" of infection (such as increased redness, warmth, or a change in the infant's feeding habits).
-
Developmental Monitoring: Corrective surgery can temporarily "pause" a child's motor milestones. Specialized pediatric physical therapists provide parents with "play-based" exercises to ensure the child regains full range of motion without putting undue stress on the repair.
Summary of Specialized Care
Specialized post-operative care is a "bridge" between a successful surgery and a thriving life. By combining the high-tech monitoring of the NICU with the biological precision of Silicone Stabilization and Thermal Management, medical teams in Riyadh ensure that the correction of Congenital Anomalies is permanent and aesthetically harmonious. The focus remains on a "silent" recovery—where the infant is kept comfortable, the tissues are kept hydrated, and the growth of the child is never hindered by the surgical past. Through these medically optimized frameworks, the journey of healing becomes a foundation for a future characterized by health, symmetry, and total confidence.